This is Kim Snyder, Associate at ICF International, Rene Lavinghouze, Evaluation Team Lead for CDC’s Office on Smoking and Health, and Patricia Rieker, Adjunct Professor of Sociology at Boston University and Associate Professor of Psychiatry at Harvard Medical School. We have been investigating public health program infrastructure as an ignored component of the left hand side of logic models.
Evaluators often are asked to focus on outcomes or the right hand side of the logic model. How often is life better for people because of a successful public health program (e.g. fewer heart attacks, less exposure to second hand smoke)? While we value the importance of this type of evaluation, we were concerned that the inputs or foundation of our activities are not fully understood. If we don’t start out with the foundation that enables organizational capacity, how are we supposed to really know what affects the outcomes on the right side of logic models?
Lesson Learned:
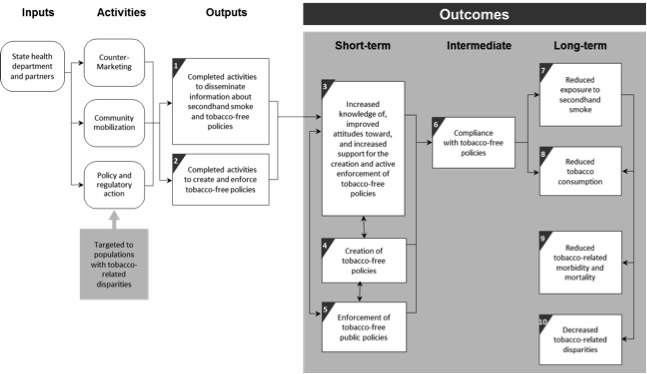
- The left hand side of the logic model is something that is rarely defined or explained in public health programs. Take a look at the Office on Smoking and Health’s logic model for eliminating nonsmokers’ exposure to secondhand smoke. Under Inputs, what is meant by “State health department and partners”? If it is interpreted and replicated differently can we expect the same outcomes?
So we decided it was important to define and study what functioning public health program infrastructure (or the foundation of public health outcomes) looks like. Previous work, a literature review across public health programs (see Rad Resource) and data from 19 tobacco control programs were used to further our understanding of functioning program infrastructure.
Building on previous work (that is currently in press with the Journal of Public Health Management & Practice) we define infrastructure as a key component and the foundation or platform that supports capacity, implementation, and sustainability of program initiatives; a definable entity, a cyclical process and part of a larger system that requires constant vigilance to be effectively maintained. Using a grounded theory approach we developed the Component Model of Infrastructure or CMI for short.
Rad Resource: Infrastructure: More Than Platforms For Moving Vehicles available in the American’ Evaluation Association (AEA) Public eLibrary.
Sneak Peek:
We are still refining the CMI and hope to share a final version this year. We define five core components of public health program infrastructure:
- Networked Partnerships,
- Multi-Level Leadership,
- Engaged Data,
- Managed Resources, and
- Responsive Plans/Planning.
We see the CMI as a practical model of public health program infrastructure that could provide the framework that grant planners, evaluators, and program implementers need to measure success, to link infrastructure to capacity, and to increase the likelihood that health achievements will be sustainable.
Do you have questions, concerns, kudos, or content to extend this aea365 contribution? Please add them in the comments section for this post on the aea365 webpage so that we may enrich our community of practice. Would you like to submit an aea365 Tip? Please send a note of interest to aea365@eval.org . aea365 is sponsored by the American Evaluation Association and provides a Tip-a-Day by and for evaluators.

If you haven’t already, I would recommend that you look at and consider the work of Renger and Titcomb. They describe a methodology for creating logic models that takes a root cause analysis approach to better defining outcomes and the “left side of the logic model”. Their approach helps reveal and clarify the sometimes hidden left side stuff.
You can find a copy of their article here: http://goo.gl/YlAfV
I hope this helps.
-BB
Rotate the logic model template by 90 degrees and you have the basis for self-evaluating one’s capacity to create them.
Best,
Chad