Hi! I’m Shannon Campbell, senior research/evaluation analyst for Multnomah County’s Mental Health and Addiction Services Division (MHASD). Beyond its responsibilities as the local mental health authority, MHASD also partners with Health Share of Oregon to co-manage Medicaid behavioral health benefits.
Recognizing the links between physical and behavioral health, reducing emergency department (ED) visits, is an important outcome for many of our programs. I recently analyzed how substance use and mental health intersect with ED visits for our Medicaid population—a dataset of 270,000 visits over 3.5 years. This first analysis was intended as a foundation for future work—to get the ‘big picture’ of what was happening in our hospitals, and later connect that data to our clients and services.
The first, most simple approach would be to calculate how many visits claimed behavioral health diagnoses. However, this approach may be insufficient if our goal is to understand not only the obvious links between behavioral and physical health (e.g., overdoses or psychoses), but also the more subtle—for example, if someone is admitted for something that could be addiction-connected, but doctors do not take (or have) the time for standard substance use screenings, or a homeless patient presents with minor complaints in hopes of a warm bed, but their housing status is closely connected with their mental health.
Thus, approach #2: Calculate how many patients had behavioral health diagnoses in at least one ED visit, and flag those patients’ total visits that same year (e.g., if “Bob” had one 2015 visit noting alcoholism, flag all of his 2015 visits).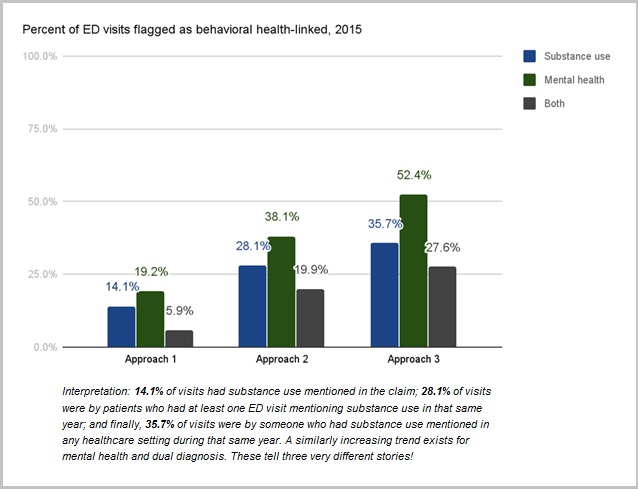
This expanded the picture further, but was it enough? I attempted one more approach: Calculate how many patients had behavioral health diagnoses in any claim (primary care, mental health services, etc.), and flag all of their ED visits [within the same year(s) the diagnosis was recorded].
Yet, when is a broken arm merely a broken arm? Is this overreach? Are we back to square one—stick with what the claim said?
The answer: Probably somewhere in-between. Further investigation is required!
Lesson Learned:
Cherry-picking methods to tell certain stories rightly deserves criticism. However, different results under different approaches can be a helpful outcome in and of itself and offers interesting new avenues of inquiry; e.g., looking at success in adopting behavioral health screening tools, the presence of specific social determinants, or what physical ailments may be signs of other underlying issues. The methods became part of the results by the questions they raised. To riff on Marshall McLuhan, sometimes the method is the message.
Hot Tip:
Find your tribe. Many of us work independently. Find people with whom you can geek out about methods, data, and the other questions you should be asking without worrying about the actual evaluation results. Bringing this project to a regional data workgroup of supportive colleagues provided great feedback, which encouraged me to reach out to my contacts more frequently to informally ‘shoot the breeze’ about current projects. Tap into your network!
The American Evaluation Association is celebrating Behavioral Health (BH) TIG Week with our colleagues in Behavioral Health Topical Interest Group. The contributions all this week to aea365 come from our BH TIG members. Do you have questions, concerns, kudos, or content to extend this aea365 contribution? Please add them in the comments section for this post on the aea365 webpage so that we may enrich our community of practice. Would you like to submit an aea365 Tip? Please send a note of interest to aea365@eval.org. aea365 is sponsored by the American Evaluation Association and provides a Tip-a-Day by and for evaluators.

I never really thought about how all these things can have an affect. I find this post to have a lot of good information to think about.